Portrait of a Pandemic: COVID-19
The world raised an eyebrow in December 2019 following the news of a “mysterious” disease outbreak in Wuhan, the capital of China’s Hubei province. Most of the 27 reported cases were workers in a seafood market in the region. Approximately 13 days later, the number of cases reached 60, and the first fatality was reported. It was later explained that a kind of coronavirus was responsible for the disease, which continued to spread rapidly, and the virus soon travelled all over the world. At the end of January, when the World Health Organization (WHO) raised the international alarm level for the disease, declaring it “a public health emergency”, the other eyebrow was also raised.
While the total number of cases and deaths were buzzing around in the air, several countries started implementing different restrictive measures. Travel bans, curfews, closed schools and workplaces, cancelled events and conferences, suspended sports competitions, quarantined ships and cities, even whole countries going on lockdown… Despite all these measures, the virus surrounded us all. And ultimately, it entered our country as well. On the same day, WHO declared this outbreak a pandemic. So, what now?
There is at least one verified case in almost every country at the moment. How did the virus spread this much? Of course, because we have the ability to travel globally. On the other hand, the news from ground-zero stating that the number of patients started to decrease gave us some comfort. Everyone played a part in this success. We will now continue to do the same, without panic, avoiding information pollution, by listening to the warnings of experts and officials, and by heeding to these warnings with full effort.
The disease is now called COVID-19 (coronavirus disease 2019), and the virus causing it is dubbed SARS-CoV-2. It is important to give descriptive names to such diseases and the responsible pathogens. This is because viruses generally constitute crowded families, and for the sake of efficient studies, it is necessary to clearly state which member of which family we are talking about.
When we are dealing with a viral (virus-borne) disease, one of the most vital steps is to exactly identify the causing virus. Is this a virus we encountered before? Is it a different form of a previously known virus? Or are we facing a completely new pathogen? This identification is necessary to determine the strategies to be followed against the virus and the disease it causes. By clarifying the characteristics of the virus, its incubation period, the symptoms and course of the disease, how it is transmitted, how contagious it is, what to do to limit the spread potential as much as possible, a “clinical picture” of the virus can be revealed. This, in turn, helps to determine the right order of priority, the right steps, and therefore, the most effective protective strategies.
What is an epidemic, what is a pandemic? How do they spawn?
Diseases that affect a certain community living in a certain region are called “epidemics” in the medical language. If the disease spreads to more than one continent, or to the entire world, then it may be defined as a “pandemic”. However, not every globally-common disease gets to be called a pandemic. There is an additional condition: the disease must be infectious and contagious.
Such diseases do not just “self-create”, of course. One of the reasons for their spawning is the opening of new habitats. When we destroy natural areas for various purposes such as agriculture or settlement, we can be exposed to pathogens we never encountered before.
Another spawning pool is a place where different animal species that do not normally coexist in nature are kept together for a long time. For example, farms where different types of livestock are raised together. China’s famous “wet markets” are, of course, another great example. Such environments are, in a sense, pathogen hatcheries. Viruses are generally specific to certain animal classes. But in such places, they start mutating in order to jump to other species, ones they do not normally encounter. When the mutation in question is achieved, and the humans are included in the equation, you are bound to have a brand new epidemic in your hands.
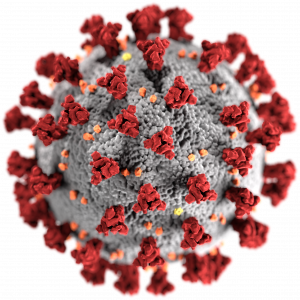
What do we know about the coronaviruses?
The name of the coronavirus family, which includes diseases such as SARS and MERS, comes from their sun-like shapes. The word “corona” means “crown” in Latin. Scientists examining these viruses under electron microscopy saw the club-like protruding proteins on the layer covering the surface of virus particles and thought they resembled the Sun’s corona.
Coronaviruses are RNA viruses that are considered large among their own ranking. But they’re still too small to see without a microscope. They are air-borne (meaning transported in the air), similar to the influenza virus, and are transmitted through the uptake of viruses either floating in the air or adhering to surfaces. They are all considered zoonotic (of animal origin) and cause diseases in mammals and birds. Not all of them are lethal, some only cause mild upper respiratory infections. But some like SARS, MERS, and Covid-19 can sometimes be lethal.
What about the new coronavirus?
Like the other members of its family, SARS-CoV-2 primarily affects the upper respiratory tract, and happily replicates there. But its main target is the lungs. Studies show that it may as well cause very mild symptoms in some people, or even, no symptoms at all (if you are the extremely lucky 1 person in a hundred).
The disease begins like an ordinary cold: with a dry cough, fever, muscle pain (myalgia), and fatigue. In some cases, the picture gets worse by the second week. Lung infections, pneumonia, difficulty in breathing, and oxygen deficiency (hypoxemia) may occur. It is also reported that nausea, vomiting, and diarrhoea can be seen in some people.
A site prepared by the CSSE of Johns Hopkins University shows regularly updated numerical data on COVID-19 cases worldwide. According to the site, the disease currently has a mortality rate of around 3.6 percent. This is quite low compared to other outbreaks the world survived in the past. A simple comparison you may find in a number of sources: According to the estimates of WHO, the SARS epidemic in 2003 had a mortality rate of around 9.6%, and this rate was 35% for MERS. However, the slow course of COVID-19’s clinical picture, or the absence of serious symptoms for a relatively long time, prevent being alarmed promptly and thus is accepted as a feature increasing the disease’s rate of spreading.
On another note, you may take a look at the electron microscope photographs of the new coronavirus and some visual models based on them, on the Flickr page prepared by the Rocky Mountain Laboratories of the US National Institute of Allergy and Infectious Diseases.
How is it transmitted?
The relatively large size of coronaviruses compared to other airborne viruses works for our advantage. This way, they are not able to float around happily in the air for a long time or move beyond a few meters. Probably thanks to this characteristic, they do not infect everyone inside an aircraft during a short flight. But of course, they can go much further with particles sprayed from the mouth and nose when we cough or sneeze –sometimes even when we talk or laugh.
The transmission generally occurs in two ways: 1) by direct exposure to airborne particles, or 2) by touching one’s mouth, nose, and eyes after hand-contact with infected surfaces. One case from Hong Kong where a dog was tested weakly positive for the new coronavirus raised concerns about people transmitting the virus to their pets, but this possibility was overruled when blood samples from the dog revealed no viral genetic substance.
The genetic analyses show us that the coronavirus we are currently dealing with has a 96% genetic similarity to the coronavirus strains seen in bats. As a matter of fact, the coronavirus responsible for the SARS epidemic had also originated from bats, then was passed on to palm civets, and from there to humans. Another study published in February stated that the new coronavirus and the coronaviruses seen in pangolins have a 99% genetic similarity, suggesting that pangolins may have served as intermediate hosts in this epidemic.
Who is at higher risk?
In general, the body’s resistance to diseases decreases with age. The same is true for COVID-19. Regardless of age, people with weakened or suppressed immune systems (due to various reasons), as well as people with certain secondary illnesses such as diabetes, heart and lung diseases, are generally more susceptible to viral diseases.
Both the transmission and mortality rates are very low for kids and teenagers, until the age of 18. The youngest patient reported was a 30-hour-old baby born in Wuhan Hospital, to an infected mother. On the other hand, in another part of China, a mother diagnosed with COVID-19 gave birth to a perfectly healthy baby, eliminating the possibility that the virus will definitely be transmitted from mother to baby.
Still, no one should act fearless and ignorant thinking “I am young and I have a killer immune system.” This is valid for all diseases, not just Covid-19. Young and healthy people play a much more active role in spreading the virus, as they visit crowded areas and participate in crowded events more frequently. Therefore, for the sake of general public health, they probably constitute the most important segment that should comply with the warnings.
Another set of data suggests that men tend to have a higher rate of susceptibility to this virus. The same was true for both SARS and MERS. Although the reason is not yet scientifically clarified, experts think it might have to do with the fact that men are more likely to smoke and take poorer care of their health.
Why 14 days?
According to a study conducted by Johns Hopkins Bloomberg School of Public Health, which used 181 cases of positive infection from outside of China’s Hubei region (reported and approved before February 24), it takes an average of 5 days for the first symptoms to appear after exposure to the virus. However, the dataset giving this average has 2 days on one end and 11 days on the other.
The same study suggests that this period can be extended up to 14 days within more protective assumptions. For this reason, the quarantine period is specified and agreed on as 14 days. Of course, there is the possibility of not being infected as soon as a person contacts the virus. The researchers also point out that, in extreme cases, longer monitoring times may be required. But for now, the gold standard is 14 days.
What should we be careful about?
In fact, the things we need to be careful about are not just specific to this disease. What we need to do to protect ourselves against pathogens, in general, is always the same.
The highest priority goes to strengthening the body’s immune system and keeping it strong. Sleeping properly, eating properly, avoiding substances that can harm the body, keeping the body active, and taking care of hygiene. Let’s elaborate on a few of them.

If you want to take it a step further, you may prefer the N95 type respirators shown in the photo. All masks should be worn to cover both the mouth and the nose. But even if you use the most protective of all masks, you should keep your possibly-infected hands away from your eyes. The awareness of proper nutrition is pleasantly increasing in many parts of the world. The notion of buying everything “in its season” and consuming different food groups in good balance, more or less, became common. We have finally learned that animal source foods may carry more pathogens, and thus should be cooked well. Although sometimes regarded as a matter of preference, it is strongly recommended to cook meat and eggs well during an outbreak like this.
As for hygiene, we need to advance a little faster, globally. Closing our mouth when coughing or sneezing, and doing this with the inside of our elbow instead of our hands, is still something we could not quite get accustomed to. We seem to be doing much worse when it comes to paying attention to not being in crowded places, including public transport, anytime we are sick. Very few of us stay home and rest, or wear a mask if we need to go to a hospital. The things mentioned in this paragraph make up the most critical spreading cause for diseases, from person to person and even from country to country, as seen in the Covid-19 example.
Hand hygiene is a valid and essential method of prevention for all infectious diseases. Because every single day, our hands contact a number of things and literally collect pathogens from surfaces. When those hands touch our mouth, nose, or eyes, the pathogen gets a free pass into our bodies. Door handles, windows, telephones, computer keyboards, light and elevator buttons, money, credit cards… These places where the hands of multiple individuals touch are the ideal contamination environments. Frequent washing of hands is the best solution, not only when there is an epidemic, but at all times. However, experts advice to dry hands with towels or paper towels, not with hot air machines. Proper cleaning of various surfaces twice a day completely eliminates the coronaviruses, as proven by a study.
In case of an epidemic, for the sake of feeling more comfortable, you can prefer soaps, sprays and surface cleaners with a wider spectrum of disinfecting properties. However, remember to read the labels before using these products; antibacterial properties only protect against bacteria, and you should look for high alcohol content or antiviral properties if you need to protect yourself against viruses. It may also be wise to use latex gloves to protect hands in certain situations -provided that you do not touch your mouth, nose, or eyes with those.
Finally, as with any epidemic, it is necessary to compromise traditional forms of warm greetings for a certain period of time. Although remote greetings are not really a part of Turkish culture, there is no doubt that it considerably reduces the risk in such cases.
Is there a treatment?
Not yet. Studies on developing a vaccine began very quickly, thanks to Chinese researchers who sequenced the virus’ genes. Unfortunately, mass producing a vaccine on a global scale usually cannot progress too quickly. This is because you need to ensure (and assure) that the vaccine you produced is both effective and safe. You need to make a lot of trials and may need to go back to the design stage if the results are not promising. If all goes well, you apply for the necessary permits, and only upon receiving these permits, you may mass-produce your vaccine. Therefore, in diseases like COVID-19, the outbreak usually fades out until a vaccine is on the shelves. And of course, it is always a possibility that the virus may mutate in the meantime, and return to us in a different form. This means, in a sense, returning to the starting point or somewhere very close to it.
Experts agree that it will take at least a year until an effective vaccine is commercially available.
For more information about COVID-19, you may visit the relevant site of the Turkish Ministry of Health or the page prepared by Koç University.
[/vc_column_text][/vc_column][/vc_row]
REFERENCES
- 1. https://www.who.int/health-topics/coronavirus
- 2. https://www.nature.com/articles/s41564-020-0695-z
- 3. https://foreignpolicy.com/2020/01/26/2019-ncov-china-epidemic-pandemic-the-wuhan-coronavirus-a-tentative-clinical-profile/
- 4. https://annals.org/aim/fullarticle/2762808/incubation-period-coronavirus-disease-2019-covid-19-from-publicly-reported
- 5. https://www.theguardian.com/world/2020/mar/10/can-face-mask-stop-coronavirus-covid-19-facts-checked
- 6. https://medicalxpress.com/news/2020-03-coronavirus-lingers-rooms-toilets-disinfectants.html
- 7. https://www.theguardian.com/world/2020/feb/05/coronavirus-mother-baby-transmission-unproven-despite-case-of-newborn
- 8. http://www.xinhuanet.com/english/2020-02/03/c_138752711.htm
- 9. https://www.nature.com/articles/d41586-020-00364-2
- 10. https://www.nature.com/articles/d41586-017-07766-9
- 11. https://edition.cnn.com/2020/01/19/asia/china-coronavirus-spike-intl-hnk/index.html
- 12. http://weekly.chinacdc.cn/en/article/id/e53946e2-c6c4-41e9-9a9b-fea8db1a8f51
- 13. https://www.businessinsider.com/coronavirus-cases-why-more-men-than-women-2020-2
- 14. https://www.washingtonpost.com/business/energy/chinese-food-will-determine-the-spread-of-pandemics/2020/01/22/a2b901fc-3d95-11ea-afe2-090eb37b60b1_story.html
- 15. https://www.sciencealert.com/uk-team-tests-china-virus-vaccine-on-mice
